Gut microbiota depletion by chronic antibiotic treatment alters the sleep/wake architecture and sleep EEG power spectra in mice
(Published Nov 11, 2020)
The intestinal environment, including the gut flora, has been shown to interact with brain function.
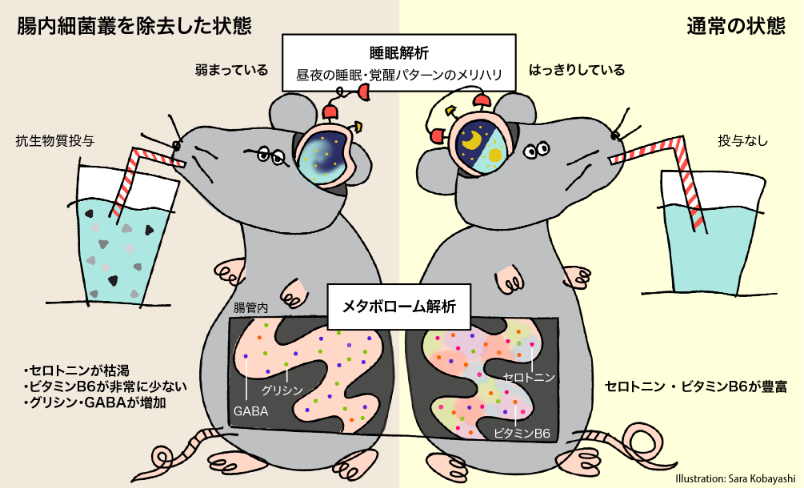
In this study, the relationship between the intestinal flora and sleep was investigated using mice in which the intestinal flora was removed by chronic antibiotic administration. A metabolome analysis of the contents of the cecum determined that the state of intestinal metabolism in “intestinal flora-removed” mice showed significant changes in the metabolic pathways of amino acids involved in neurotransmitter synthesis compared to normal mice. In particular, vitamin B6 was significantly reduced and serotonin, which regulates nerve function, was depleted.
On the other hand, a significant increase in glycine and gamma-aminobutyric acid (GABA), which suppress the activity of nerve cells, was observed.
When sleep was analyzed using EEG and EMG, “intestinal flora-removed” mice had decreased sleep in the light period (sleep period) and increased sleep in the dark period (active period). The day and night, sleep / wakefulness pattern was weakened. It was also found that theta waves, which are the characteristic brain waves components of REM sleep with cerebral cortex activity, were reduced. These findings suggest that removal of the gut flora may reduce sleep quality.
It is expected that further research may allow new methodologies for promoting improved health through a deeper understanding of the interaction between the intestinal environment and brain function (gut-brain axis) and eating habits.